Many of us are familiar with back pain, which disrupts normal life for a long time. Although the cause may be trauma, neurological diseases or malformations of the spinal column, osteochondrosis of the lumbar spine often becomes a provocateur of unpleasant sensations. This degenerative disease can occur even at a young age, its initial manifestations can be detected even in adolescents and schoolchildren, but the bulk of patients are people after 40 years. Changes in the spinal column associated with osteochondrosis can occur in any part, from the cervical to the lumbar and sacrococcygeal. But the most common form that brings patients a lot of unpleasant and painful sensations is osteochondrosis of the lumbar spine. What kind of pathology is this, what is characteristic for it and does the pain in the lower back always speak about this disease.
Osteochondrosis of the lumbar spine: what is the essence of the pathology?
Osteochondrosis is a term derived from two words: the Greek osteon, which means bone, and chondron, which is cartilage. Thus, osteochondrosis of the lumbar spine (and all others, too) is initiated by changes in the cartilage of the discs, which are a natural "lining" between the vertebrae and the shock absorber during movement. Changes in the structure of the disc and its functionality are accompanied by a natural reaction in the vertebral body. With this disease, degenerative changes gradually occur in the body of the discs. The height of the disc decreases, due to which its physiological function is lost, causing instability and changes in the vertebral joints. As the disease progresses, a reaction occurs in the endplate of the vertebral body. This reaction can be divided into three stages: edema due to malnutrition and dystrophic changes, fatty degeneration and, at the last stage, sclerosis.
Causes of osteochondrosis of the spine
Our vertebral discs begin to gradually deform and change when we are about 20 years old. The gradual decrease in fluid within the disc body leads to a decrease in the size of the space between the vertebrae (chondrosis). This means that the disc can no longer function as a shock absorber and the tension in the anterior and posterior longitudinal ligaments of the vertebrae changes. As a result, a much greater load is imposed on the vertebral joints, which increases from year to year. The spinal ligaments are not positioned correctly and are unevenly stretched, and the movable segments of the spine gradually become unstable. The dorsal segment usually consists of two adjacent vertebral bodies and a disc between them. The upper and lower end plates in the vertebral body are subjected to more stress, thickening zones (sclerosis) and ridges at the borders (spondylophytes) gradually develop. Due to such changes, the entire clinical picture of the disease is formed in the future.
What are the symptoms of osteochondrosis of the lumbar spine?
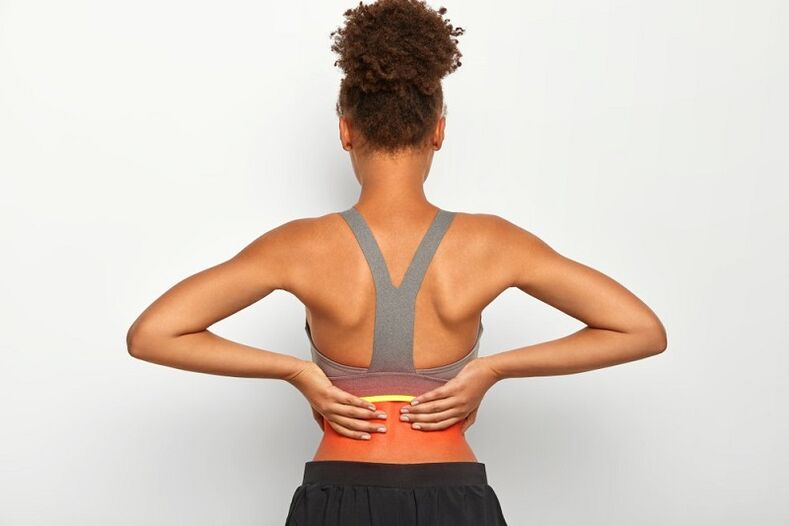
Almost any form of the disease manifests itself in the form of excruciating back pain, which is difficult to control and which affects a specific segment of the spine (from the neck to the lower back and sacrum). Symptoms of osteochondrosis of the lumbar spine may remain limited only to the spine (in the lumbar region) or spread to the legs if they come from the lumbar spine, or the arms if they come from the cervical spine.
Symptoms may occur during rest, exertion, or habitual activity. There may be radicular symptoms caused by compression, irritation in the area of the nerve root, or pseudo-radicular symptoms if the cause is in the facet joint or adjacent muscles. Often, osteochondrosis of the lumbar spine is combined with lesions in other areas - the thoracic, cervical spine - then the symptoms will be wider. In other words, discomfort and pain provokes not only one segment that is damaged, but several areas of osteochondrosis at once. The disease has an undulating course with periods of exacerbations (symptoms can seriously interfere with normal life) and temporary remissions, when the manifestations diminish or almost disappear. But any factors, physical or mental, can lead to a sudden relapse.
How is spinal osteochondrosis diagnosed?
The diagnosis is based on the study of the patient's medical history and complaints, physical examination with the identification of typical symptoms and neurological examination. Today, doctors are increasingly inclined to perform instrumental diagnostics, since other pathologies are often hidden under the guise of osteochondrosis.
For example, among patients suffering from persistent back pain and planning surgery to relieve pain, bone health is an important factor. If a patient is found to have low bone density before surgery, this may affect the treatment plan for osteochondrosis before, during and after the procedure. A study from the Hospital for Special Surgery (HSS) in New York showed that computed tomography of the lumbar spine before surgery showed that a significant number of patients had low bone density that had not been previously diagnosed.
Almost half of the nearly 300 patients tested were diagnosed with osteoporosis, or its precursor, osteopenia. It is especially important to take this into account at the age of over 50. The prevalence of low bone mineral density in this group was 44%, and 10. 3% were diagnosed with osteoporosis. Low bone density is a known risk factor for vertebral fractures, and this condition can be an aggravating factor in the treatment of osteochondrosis.
Treatment of osteochondrosis of the spine

Treatment options depend on the severity of your symptoms. Physical therapy is the main method of pain relief in the early stages. Ultrasound, electrotherapy, heat treatment are used. Treatment is complemented by appropriately matched pain management such as NSAIDs, muscle relaxants, and steroids. Injection practices can be used - blockades, trigger point injections. Shown are manual therapy, osteopathy, exercise therapy.
Surgical treatment is always the last resort. There are situations when surgery is needed. An example would be paralysis of the bladder or rectum caused by narrowing of the spinal canal or prolapsed disc, a large herniated disc. The options for the operation are selected in conjunction with the doctor. But after surgical treatment, the problem is not completely eliminated, long-term rehabilitation and lifelong supportive treatment are required. This is due to the fact that osteochondrosis does not disappear anywhere, it can progress in other departments.













































